Boston Health Care for the Homeless Will Open a Safe Room for Heroin Highs
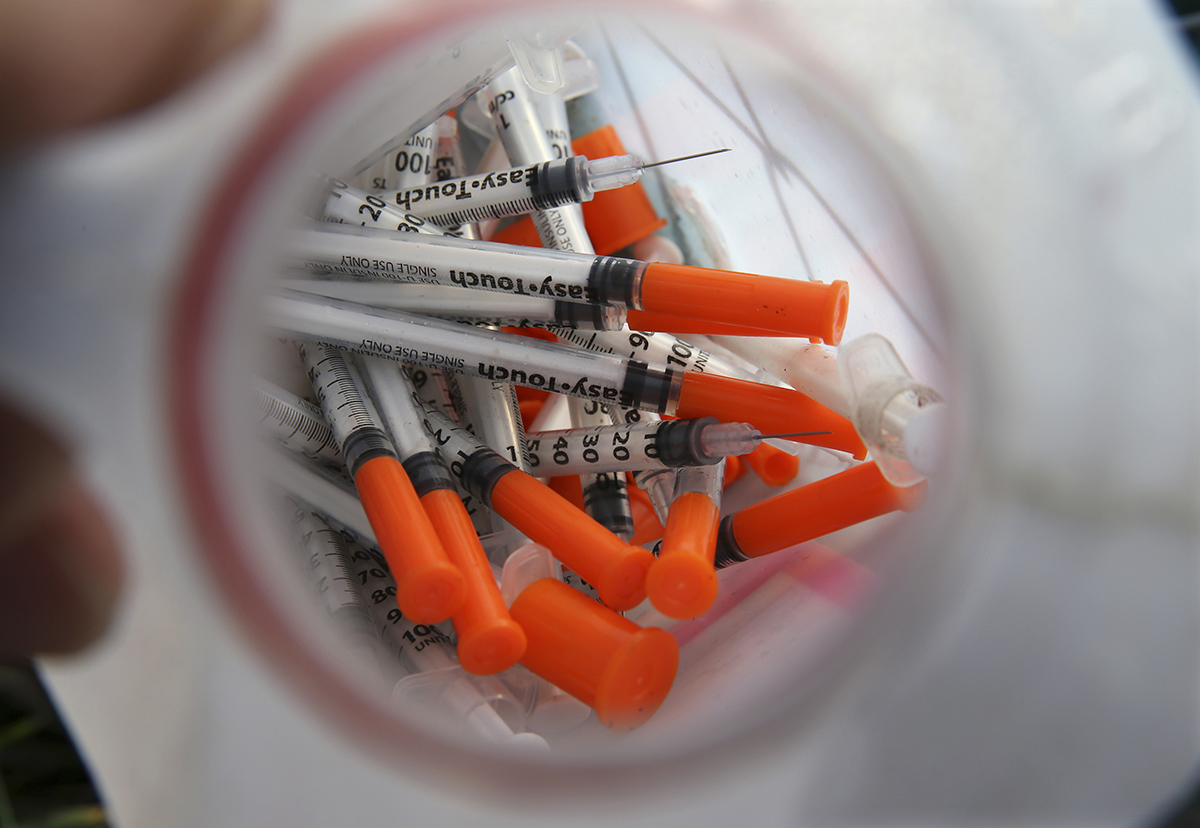
Photo via AP/Mel Evans
The Boston Health Care for the Homeless Program (BHCHP) has a new strategy to combat the opiate epidemic: a supervised safe room for heroin highs.
The small, unassuming space, located at the corner of Massachusetts Avenue and Albany Street, an area nicknamed “Methadone Mile,” is slated to open in January. It will be staffed by a nurse and an outreach worker, there to check users’ vital signs. The room will offer a refuge for up to 10 people at a time.
Responding to concerns that the space will encourage heroin use, BHCHP has stressed that the room will not be a safe injection site—that is, no drugs will be injected within the space. Rather, the staff aims to minimize the drug’s most frequent and devastating after-effects: coma, loss of breath, victimization due to theft and sexual assault, and death. All visitors will be urged to seek treatment.
Last year, the National Institute on Drug abuse reported that the number of unintentional heroin overdoses in Boston, along with several other U.S. cities, was at a decade-long high. Despite the epidemic, there are no safe injection facilities in the U.S., and this safe room is one of the first of its kind.
“It’s an important step in the direction of creating an atmosphere in which drug users can be accepted and cared for as human beings,” says Mark Eisenberg, a member of the Addictions Consult Team at Mass General’s Charlestown Health Center. “[This] does not condone drug injection, it merely recognizes that people inject drugs and will continue to do so. Even people who inject drugs deserve to be healthy, socially connected, and cared for.”
Eisenberg adds that it usually takes around five years for people struggling with substance abuse to realize they have a problem, and the safe room might help keep them alive long enough to reach sobriety.
“Offering a safe space that doesn’t stigmatize users will allow people to gain trust with the medical system until they are ready to seek treatment,” he says.
Still, this approach may not go far enough, says Joji Suzuki, a substance use psychiatrist at Brigham and Women’s Faulkner Hospital.
“It’ll get ‘jarring’ people off the street—people openly trading and nodding off on the sidewalk—but the problem is they still won’t have to safely inject,” Suzuki says. “It’s unclear what a safe space will offer without the injection component. But BHCHP is certainly headed in the right direction.”
A rep from BHCHP says the organization will not conduct new interviews until 2016.
Eisenberg and Suzuki agree that a safe injection spot in Boston would be a step in the right direction, despite a lack of political support for the idea. At a Vancouver clinic called Insite, where nurses may inject patients, the number of overdoses and needle-transmitted illnesses has greatly declined, according to Eisenberg.
“We have to think outside the box, and stop punishing people for being honest,” says Suzuki. “Otherwise, this crisis is not going away.”


